- Oak Brook:(630) 705-9999
- Chicago:(312) 920-8822
- Email:inquiry@vervecollege.edu
- Make a Payment
- Home
- Programs
- Admission
- Resources
- ATI Entrance Exam Resources
- New E-Digital Library
- Refer a Friend
- School Newsletter
- Events
- Employers
- Job-Network
- Alpha Beta Kappa Candidates
- Verve College Library
- Graduation and Pinning Ceremony Photo Galleries
- Textbook Information
- Career Services
- Tutoring
- School Catalog
- FAQ
- Constitution Day Program
- Alumni
- Verve College Plans
- Financial Aid
- HEERF Reporting
- Satisfactory Academic Progress
- Apply For Financial Aid
- Net Price Calculator
- Return of Title IV Funds (R2T4)
- Financial Aid Office Code of Conduct
- Contact
- FAQs
- Verification Policy
- Vaccination Policy
- Student Right-to-Know Act
- Misrepresentation
- Information Security Program
- Academic Award Year
- Availability of Employee
- Cost of Attendance
- Health & Safety Exemption Requirement
- Students Rights and Responsibilities
- Leave of Absence
- Pell Formula
- Military Students
- Grants/ Scholarship Policy
- Contact Us
- Testimonials
- Blog
Is a Nursing Career Right For You?
Take The Free Quiz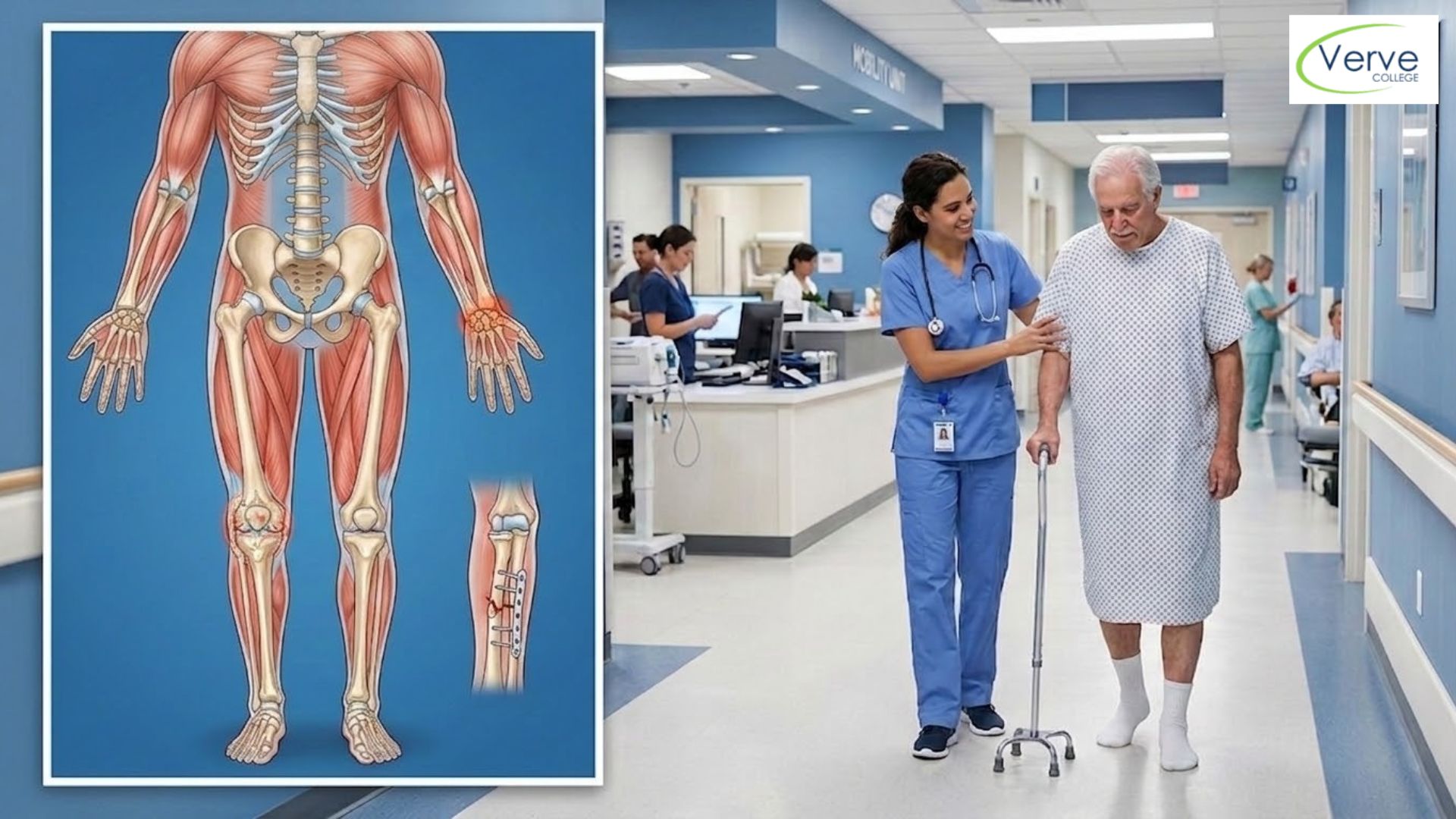
Musculoskeletal Disorders Nursing Guide: Arthritis, Fractures, and Patient Care
Musculoskeletal Disorders Nursing Guide: Arthritis, Fractures, and Patient Care
If you’re studying to become a nurse, musculoskeletal disorders will come up constantly in clinical settings. Arthritis, fractures, osteoporosis — these are some of the most common reasons patients end up in care. And yet, many nursing students feel underprepared when it comes to understanding how the bones and joints work, and what goes wrong.
This guide breaks it all down in plain language. You’ll learn how to recognize these conditions, what nursing care involves, and why building a strong foundation in body systems makes you a better, more confident nurse from day one.
Key Takeaways
- Musculoskeletal disorders nursing covers a wide range of bone, joint, and muscle conditions that nurses encounter daily
- Arthritis, fractures, and osteoporosis each require different care approaches and patient education strategies
- Knowing how the musculoskeletal system works is essential before you can assess or manage these conditions effectively
- Strong anatomy knowledge gained through anatomy and physiology classes gives you a clinical edge early in your training
- Nursing care goes beyond treatment — communication, mobility support, and pain management are equally important
- Early preparation makes clinical rotations less overwhelming and more rewarding
What Are Musculoskeletal Disorders?
Musculoskeletal disorders are conditions that affect the bones, joints, muscles, tendons, and ligaments. They range from mild (a sprained ankle) to severe (a hip fracture in an elderly patient). These conditions cause pain, limit movement, and often affect a patient’s ability to perform daily tasks.
For nurses, these aren’t edge cases. They’re everyday patient encounters. In hospitals, long-term care facilities, and outpatient clinics, musculoskeletal conditions are among the most frequently seen diagnoses.
Understanding what’s happening inside the body is the first step to giving good care.
Arthritis: Types, Symptoms, and Nursing Care
Arthritis is not one disease — it’s a term for over 100 conditions that cause joint inflammation. The two most common types you’ll encounter as a nurse are osteoarthritis and rheumatoid arthritis.
Osteoarthritis
Osteoarthritis happens when the cartilage (the cushioning between bones) breaks down over time. It’s most common in older adults and affects knees, hips, and hands. Patients experience joint pain, stiffness, and reduced range of motion.
Nursing priorities include pain management, helping patients move safely, and educating them on activity modifications.
Rheumatoid Arthritis
Rheumatoid arthritis (RA) is an autoimmune disease, meaning the body’s immune system mistakenly attacks its own joint tissue. It causes inflammation, swelling, and can affect multiple joints at once. It often appears in younger adults too.
RA patients may need help with medication management, joint protection techniques, and emotional support — because chronic pain affects mental health too.
Key Nursing Actions for Arthritis Patients
- Assess pain levels regularly using a standard pain scale
- Monitor for medication side effects, especially with long-term anti-inflammatory drug use
- Encourage gentle movement and physical therapy referrals
- Educate patients on heat and cold therapy for symptom relief
- Watch for signs of joint deformity or worsening mobility
Fractures: Recognition, Types, and Patient Care
A fracture is a break in the bone. It can be complete (bone breaks all the way through) or incomplete. Fractures are classified in several ways: closed (skin intact), open (bone breaks through the skin), stress (from repetitive force), or pathological (caused by a disease like osteoporosis).
Knowing the type of fracture helps determine the nursing care plan.
What to Assess
When a patient comes in with a suspected fracture, nurses assess for pain, swelling, bruising, deformity (visible misalignment), and loss of function. Neurovascular checks are also critical — this means checking circulation, sensation, and movement in the injured area.
Nursing Priorities for Fractures
- Immobilization: Keep the fracture site stable to prevent further injury
- Pain control: Fractures are painful. Timely pain assessment and medication administration matter
- Wound care: For open fractures, infection prevention is a priority
- Cast or splint care: Teach patients how to care for their cast and what symptoms to report
- Rehabilitation support: Encourage gradual return to function through physical therapy
Post-fracture care doesn’t end at discharge. Patient education — on weight-bearing restrictions, signs of complications, and follow-up care — is a major part of the nurse’s role.
Osteoporosis: The Silent Condition Nurses Must Know
Osteoporosis is often called a “silent disease” because bone loss happens without symptoms until a fracture occurs. It’s most common in postmenopausal women and older adults, but it affects men too.
Bones become thin and fragile, increasing the risk of fractures — especially in the spine, hips, and wrists.
Nursing Role in Osteoporosis Care
Nurses play a big role in prevention and education. Key tasks include:
- Teaching patients about calcium and vitamin D intake
- Encouraging weight-bearing exercises to maintain bone density
- Assessing fall risk and recommending home safety modifications
- Monitoring medications like bisphosphonates (drugs used to slow bone loss) and their side effects
- Identifying patients at risk before a fracture happens
Fall prevention is one of the highest-impact things a nurse can do for a patient with osteoporosis.
Why Body Systems Knowledge Matters in Musculoskeletal Care
You can’t assess what you don’t understand. If you’re not clear on how bones grow, how joints are structured, or how muscles attach and function, it’s hard to recognize when something is wrong.
This is why nursing educators consistently emphasize foundational science. Many students pursuing lpn programs find that the students who thrive in clinical settings are the ones who invested time in understanding anatomy before entering the clinical floor.
Knowing that the femur is the body’s longest bone, or that synovial fluid lubricates joints, isn’t just trivia. It directly informs how you assess a patient and communicate with the care team.
Common Misconceptions Students Have About Musculoskeletal Nursing
One of the biggest mistakes new students make is thinking musculoskeletal care is mostly about bones and casts. In reality, it’s deeply about the patient as a whole.
Chronic musculoskeletal conditions affect mood, independence, and identity. A patient with severe arthritis may be grieving the loss of hobbies they loved. A fracture patient may fear losing their independence. Nurses who understand this provide better, more human care.
Another misconception is that musculoskeletal conditions only affect elderly patients. While age increases risk, these disorders affect people across all age groups — from sports-related fractures in teenagers to autoimmune arthritis in young adults.
Practical Steps to Prepare for Musculoskeletal Nursing
Here’s how to get ahead:
Start with the science. Before clinical rotations, strengthen your understanding of how the skeletal and muscular systems work together. This makes everything else click faster.
Practice patient communication. Patients with chronic pain are often frustrated or anxious. Role-playing difficult conversations during training helps you respond calmly and effectively.
Learn the medications. NSAIDs, corticosteroids, bisphosphonates — know what they do, why they’re used, and what side effects to monitor for.
If you’re looking for accredited lpn programs that include real clinical experience and structured curriculum support, Verve College in Illinois offers programs designed to prepare you for exactly these kinds of patient encounters.
Conclusion
Musculoskeletal disorders are a core part of nursing practice. Whether you’re caring for a patient recovering from a hip fracture or helping someone manage daily pain from rheumatoid arthritis, the knowledge and compassion you bring matters.
Start with a strong foundation in anatomy, learn to assess carefully, and always treat the whole patient — not just the bone or joint. Understanding musculoskeletal disorders nursing now puts you steps ahead in your training and your career.
If you’re preparing for nursing school or looking to build your clinical confidence, the right education makes all the difference.
Get Your Nursing Career Training Readiness Score Now!
FAQs
What does a nurse do for patients with musculoskeletal disorders?
Nurses assess pain, monitor mobility and function, administer medications, educate patients on self-care, and support rehabilitation. They also watch for complications like infection (in fractures) or medication side effects (in arthritis management). The role combines clinical skill with strong patient communication.
I don’t have a science background. Will I struggle with musculoskeletal content in nursing school?
It can feel overwhelming at first, but it gets easier with the right preparation. Taking foundational courses in anatomy and physiology before starting your nursing program can make a significant difference. Many students use prep classes to build confidence before clinical training begins.
How do I know if an LPN program will prepare me for musculoskeletal nursing care?
Look for programs that include hands-on clinical training and a structured curriculum covering medical-surgical nursing topics. Accredited programs from recognized bodies like ABHES typically cover musculoskeletal conditions as part of core clinical training. Verve College, for example, includes clinical experience that prepares students for real patient care scenarios from the start.
 Sign up
Sign up Login
Login