- Oak Brook:(630) 705-9999
- Chicago:(312) 920-8822
- Email:inquiry@vervecollege.edu
- Make a Payment
- Home
- Programs
- Admission
- Resources
- ATI Entrance Exam Resources
- New E-Digital Library
- Refer a Friend
- School Newsletter
- Events
- Employers
- Job-Network
- Alpha Beta Kappa Candidates
- Verve College Library
- Graduation and Pinning Ceremony Photo Galleries
- Textbook Information
- Career Services
- Tutoring
- School Catalog
- FAQ
- Constitution Day Program
- Alumni
- Verve College Plans
- Financial Aid
- HEERF Reporting
- Satisfactory Academic Progress
- Apply For Financial Aid
- Net Price Calculator
- Return of Title IV Funds (R2T4)
- Financial Aid Office Code of Conduct
- Contact
- FAQs
- Verification Policy
- Vaccination Policy
- Student Right-to-Know Act
- Misrepresentation
- Information Security Program
- Academic Award Year
- Availability of Employee
- Cost of Attendance
- Health & Safety Exemption Requirement
- Students Rights and Responsibilities
- Leave of Absence
- Pell Formula
- Military Students
- Grants/ Scholarship Policy
- Contact Us
- Testimonials
- Blog
Is a Nursing Career Right For You?
Take The Free Quiz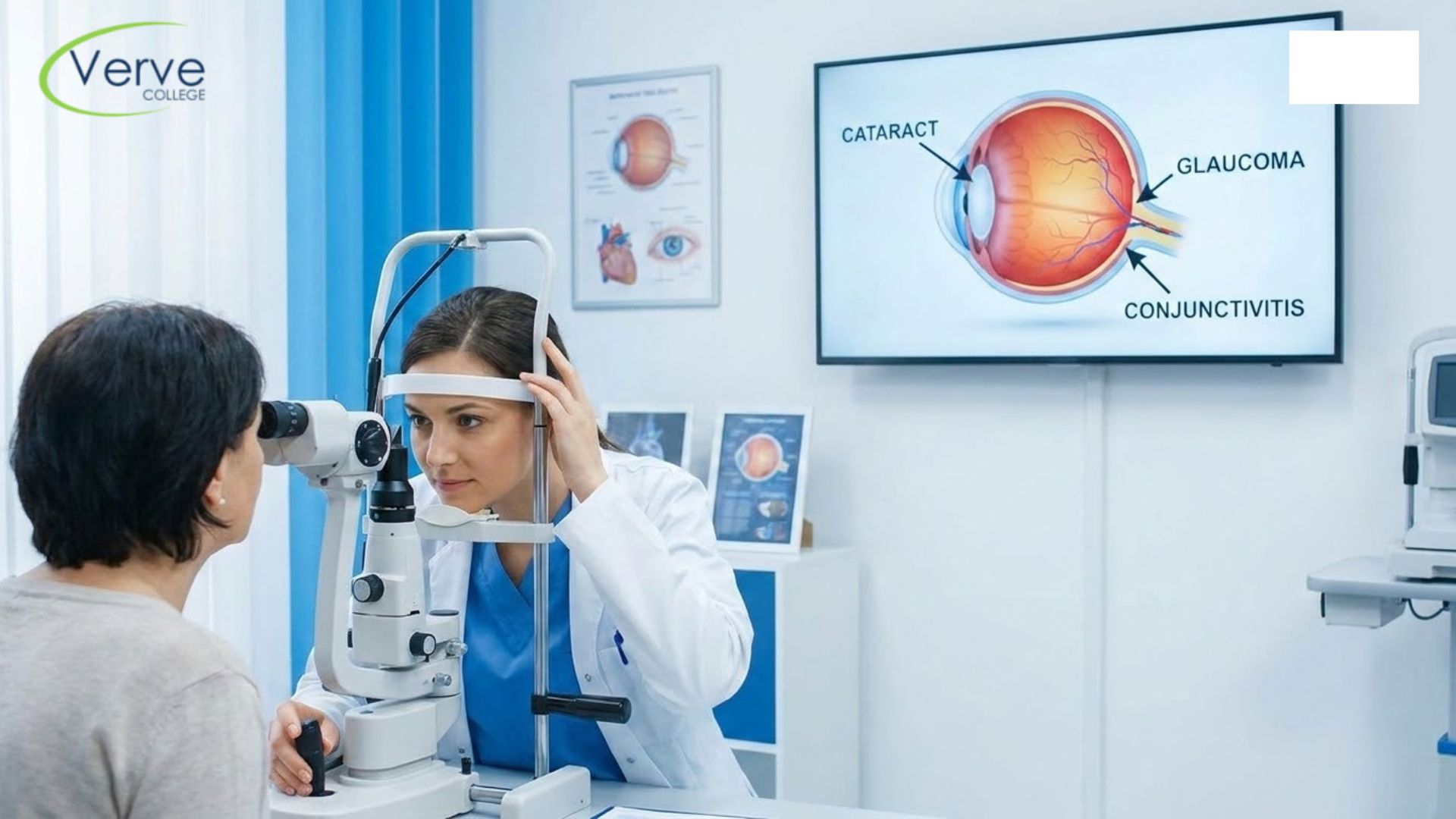
Common Eye Disorders in Nursing | Symptoms and Patient Care
Common Eye Disorders in Nursing | Symptoms and Patient Care
Most nursing students spend a lot of time thinking about the heart, lungs, and vital signs. Eye health often gets less attention, but it shouldn’t. Visual changes can be early signs of serious systemic conditions, and recognizing them quickly can make a real difference for your patient.
Eye disorders nursing is not just for ophthalmology specialists. Every nurse, regardless of setting, needs a basic ability to recognize common eye conditions, understand what they signal, and know when something needs urgent attention.
This guide breaks down the conditions you are most likely to encounter, the assessment skills that matter, and how your foundational training sets you up to handle them with confidence.
Key Takeaways
- Many common eye disorders show up in general nursing settings, not just specialty clinics
- Recognizing the difference between urgent and non-urgent eye symptoms is a core nursing skill
- Conditions like glaucoma and diabetic retinopathy are directly connected to systemic diseases you will already be monitoring
- Students in anatomy and physiology classes gain the foundational knowledge of eye structure that makes clinical assessment much easier to understand
- Early documentation of visual changes can prevent permanent vision loss in some conditions
- Strong observational and communication skills are just as important as knowing the clinical facts
Why Eye Assessment Belongs in Every Nurse’s Toolkit
You do not have to work in an eye clinic to encounter patients with eye problems. A patient admitted for diabetes management may mention blurry vision. An older adult in a long-term care facility might report eye pain that turns out to be a sign of acute glaucoma. A child brought in for a routine visit might have an infection that has spread from one eye to the other.
In each of these situations, the nurse at the bedside is the first person to hear the complaint. What you do with that information matters.
Eye assessment does not require specialized equipment in most cases. It requires attention, the right questions, and the ability to tell the difference between something that can wait and something that cannot.
Common Eye Disorders You Will Encounter
Conjunctivitis
Conjunctivitis, commonly called pink eye, is one of the most frequently seen eye conditions in nursing practice. It involves inflammation of the conjunctiva, which is the thin membrane that lines the inside of the eyelid and covers the white part of the eye.
It can be caused by bacteria, viruses, or allergens. Bacterial conjunctivitis usually produces thick discharge and responds to antibiotic eye drops. Viral conjunctivitis is more contagious and clears on its own. Allergic conjunctivitis causes itching and tearing but is not infectious.
Nurses need to know which type they are dealing with because infection control protocols differ. Viral conjunctivitis spreads easily in care settings, so isolation precautions may be necessary.
Glaucoma
Glaucoma involves increased pressure inside the eye that damages the optic nerve over time. It is one of the leading causes of blindness worldwide, and what makes it particularly dangerous is that many patients do not notice symptoms until significant damage has already occurred.
Acute angle-closure glaucoma is the exception. It comes on suddenly and causes severe eye pain, headache, nausea, blurred vision, and halos around lights. This is a medical emergency. If a patient reports these symptoms, you need to escalate immediately.
Patients with chronic conditions like diabetes and hypertension are at higher risk for developing glaucoma. When you are already monitoring these patients, staying alert to visual complaints is a natural extension of that care.
Cataracts
A cataract is a clouding of the eye’s natural lens. It develops gradually and causes blurry or dim vision, increased sensitivity to light, and difficulty seeing at night. Most cataracts are age-related, though they can also develop after eye injury or as a side effect of certain medications, including long-term corticosteroid use.
Nursing care for cataract patients is most common in the post-surgical period. Cataract removal is one of the most common surgical procedures performed, and patients need clear discharge education about eye drops, activity restrictions, and signs of complications like infection or increased pressure.
Diabetic Retinopathy
Diabetic retinopathy is damage to the blood vessels in the retina caused by poorly controlled blood sugar over time. The retina is the light-sensitive layer at the back of the eye that sends visual signals to the brain.
As a nurse working with diabetic patients, you will not be diagnosing this condition. But you will be educating patients about why blood sugar control matters, encouraging regular eye exams, and documenting any reports of visual changes. These are all part of preventing irreversible vision loss.
This is a good example of why understanding body systems beyond the basics is so valuable. When you understand how hyperglycemia damages small blood vessels throughout the body, retinopathy makes sense, and so does the urgency of glycemic control.
Macular Degeneration
Age-related macular degeneration affects the central part of the retina, leading to loss of central vision. Patients describe it as a blurry or dark spot in the middle of what they see, while peripheral vision stays intact.
This condition is common in older adults, which means nurses working in geriatrics or long-term care will encounter it regularly. Safety is a major concern. Patients with central vision loss are at higher risk for falls, medication errors, and social withdrawal. Nursing care focuses on safety planning, assistive resources, and emotional support.
Retinal Detachment
Retinal detachment is a serious emergency. It happens when the retina pulls away from the tissue supporting it, cutting off its blood supply. Patients typically describe sudden floaters, flashes of light, or a curtain-like shadow moving across their vision.
If a patient reports these symptoms, do not wait. This condition requires immediate ophthalmologic intervention. Time matters because the longer the retina stays detached, the greater the risk of permanent vision loss.
What Good Eye Assessment Looks Like in Practice
You do not need a slit lamp to do meaningful eye assessment. Start with what your patient tells you. Ask about onset, whether it came on suddenly or gradually. Ask about associated symptoms like pain, discharge, or headache. Ask about any recent changes to medications or recent injuries.
Observe what you can. Look at the appearance of the eye. Note any redness, swelling, discharge, or asymmetry. Check whether the pupils are equal and reactive to light.
Document what you find clearly and report changes promptly. In conditions like glaucoma and retinal detachment, early escalation is the difference between preserving and losing vision.
Connecting the Eyes to the Rest of the Body
One of the most important things to understand about eye disorders nursing is that the eyes rarely tell a story by themselves. They are connected to systemic health in direct and measurable ways.
Hypertension can cause changes in the blood vessels of the retina. Diabetes damages small vessels throughout the body, including those in the eye. Autoimmune conditions like lupus and multiple sclerosis can cause inflammation that affects vision. Even certain medications can cause ocular side effects.
This is why students in lpn programs that cover pharmacology and body systems thoroughly are better equipped to make these connections when they get into clinical settings. You are not just treating an eye. You are looking at a whole person.
Building the Foundation Before You Specialize
Some students assume that eye care is a niche area they will only need if they end up in a specialty clinic. This is one of the more common misconceptions in nursing education.
The reality is that eye complaints, visual changes, and ocular side effects show up in every nursing environment. The nurse who can recognize the difference between a benign complaint and an emergent one is more effective, regardless of the setting.
That recognition starts with knowing how the eye works, what normal looks like, and what abnormal signals. Students enrolled in accredited lpn programs develop this kind of clinical thinking as part of their core training, not as an add-on. It is built into how you learn to assess patients from day one.
A Misconception Worth Addressing
Many students assume that if a patient’s primary complaint is eye-related, it belongs to a specialist and they should just refer and move on. That thinking can cause dangerous delays.
Your job is not to diagnose. But your job absolutely includes recognizing urgency, taking a thorough history, and making sure the right information gets to the right people quickly. The nurse who dismisses a complaint of sudden floaters and flashes as “probably nothing” may have missed a retinal detachment.
Confidence in basic eye assessment does not mean overstepping your scope. It means doing your job thoroughly and protecting your patient in the process.
Conclusion
Eye conditions show up across every care setting, and every nurse needs a working knowledge of what to look for. From conjunctivitis to retinal detachment, the range is wide, but the underlying skill is the same: observe carefully, ask the right questions, and act on what you find.
Strong nursing care is holistic care. The eyes are part of that picture, connected to the body’s larger systems in ways that matter clinically. Building this knowledge now, as part of your foundational training, puts you in a much stronger position when you are standing at a patient’s bedside.
The more you understand about the body, the more confident and capable you will be as a nurse.
Get Your Nursing Career Training Readiness Score Now!
FAQs
What eye symptoms should a nurse never ignore?
Sudden vision loss, severe eye pain, sudden floaters or flashes of light, and a shadow moving across the visual field are all symptoms that require immediate escalation. These can signal emergencies like retinal detachment or acute glaucoma, where delays in treatment can lead to permanent vision loss.
I am not going into ophthalmology. Do I really need to know this?
Yes. Eye complaints and visual changes come up in general medical, geriatric, diabetic, and pediatric care settings regularly. Knowing how to assess them and when to escalate is part of being a competent generalist nurse, regardless of your specialty focus.
How do I start preparing for eye assessment as a nursing student?
Start with your anatomy and physiology content. Understanding the structure of the eye and how it connects to other body systems makes clinical content easier to retain. From there, practice taking focused histories and learning to describe what you observe clearly and precisely. These habits carry over into every area of nursing practice.
 Sign up
Sign up Login
Login