- Oak Brook:(630) 705-9999
- Chicago:(312) 920-8822
- Email:inquiry@vervecollege.edu
- Make a Payment
- Home
- Programs
- Admission
- Resources
- ATI Entrance Exam Resources
- New E-Digital Library
- Refer a Friend
- School Newsletter
- Events
- Employers
- Job-Network
- Alpha Beta Kappa Candidates
- Verve College Library
- Graduation and Pinning Ceremony Photo Galleries
- Textbook Information
- Career Services
- Tutoring
- School Catalog
- FAQ
- Constitution Day Program
- Alumni
- Verve College Plans
- Financial Aid
- HEERF Reporting
- Satisfactory Academic Progress
- Apply For Financial Aid
- Net Price Calculator
- Return of Title IV Funds (R2T4)
- Financial Aid Office Code of Conduct
- Contact
- FAQs
- Verification Policy
- Vaccination Policy
- Student Right-to-Know Act
- Misrepresentation
- Information Security Program
- Academic Award Year
- Availability of Employee
- Cost of Attendance
- Health & Safety Exemption Requirement
- Students Rights and Responsibilities
- Leave of Absence
- Pell Formula
- Military Students
- Grants/ Scholarship Policy
- Contact Us
- Testimonials
- Blog
Is a Nursing Career Right For You?
Take The Free Quiz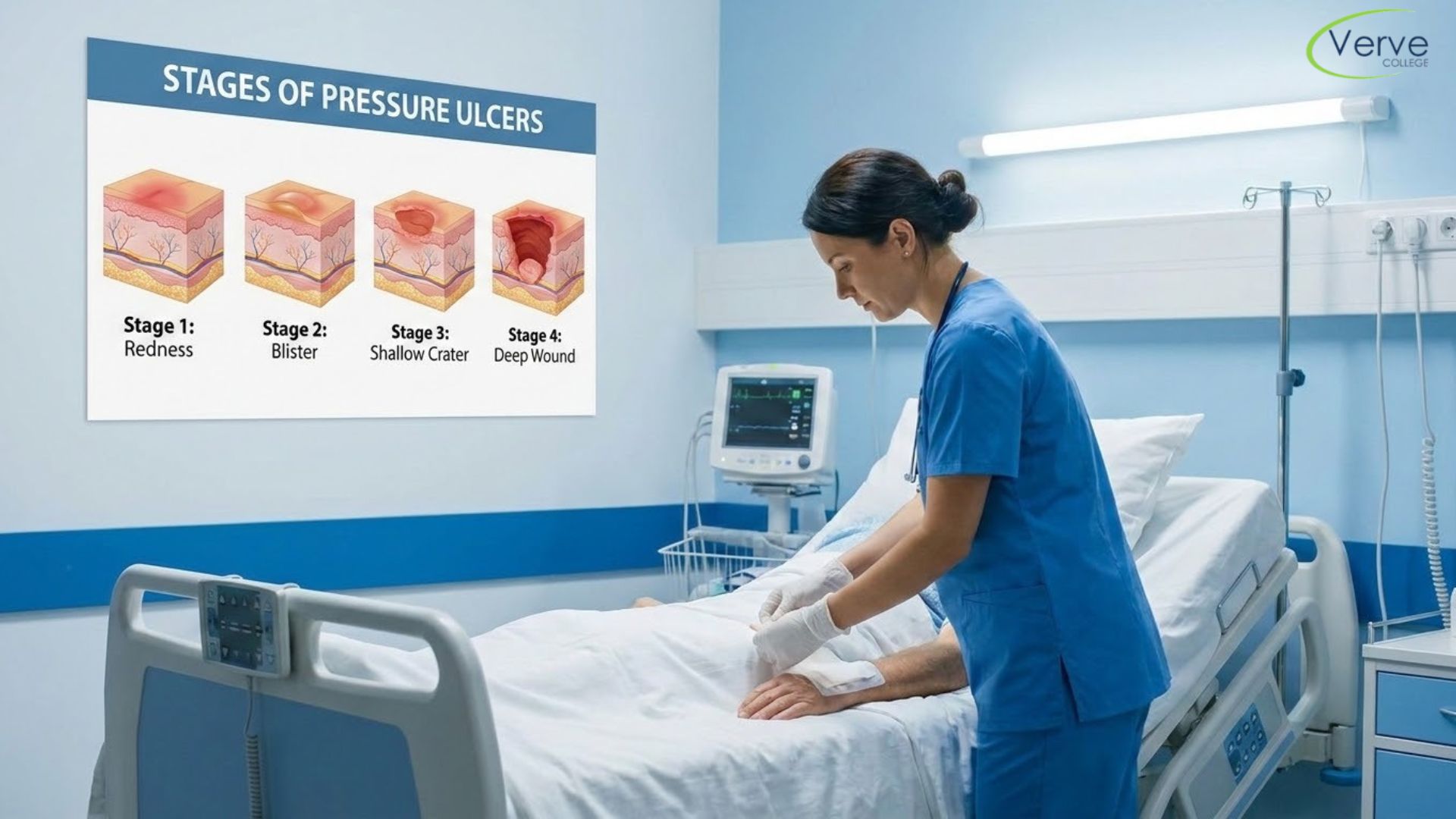
Pressure Ulcer Staging and Prevention: A Nursing Care Guide
Pressure Ulcer Staging and Prevention: A Nursing Care Guide
Pressure ulcers are one of the most preventable complications in patient care, yet they remain a serious problem across hospitals, nursing homes, and home health settings. For LPNs, knowing how to identify, stage, and prevent them is not optional — it is a core clinical skill.
This guide walks you through pressure ulcer staging in nursing, what each stage means, how to prevent breakdown before it starts, and what your role looks like on the care team.
Key Takeaways
- Pressure ulcers develop when sustained pressure cuts off blood flow to the skin and tissue underneath
- There are four official stages, plus two additional categories used in clinical settings
- Early identification is everything — catching a Stage 1 ulcer prevents it from becoming a Stage 3 or 4
- Prevention involves repositioning, skin assessment, nutrition, and moisture control
- LPNs play a central role in both prevention and ongoing wound monitoring
- Students in lpn programs learn skin integrity and wound care as part of their core clinical training
What Is a Pressure Ulcer and Why Does It Happen?
A pressure ulcer, sometimes called a bedsore or decubitus ulcer, forms when pressure is applied to an area of skin for too long. That pressure restricts blood flow, and without blood, tissue begins to break down.
They most commonly develop over bony prominences — areas where bone sits close to the surface of the skin. Think heels, sacrum (the tailbone area), hips, elbows, and the back of the head.
Patients who are bedridden, use a wheelchair, have limited mobility, or cannot feel pain are at the highest risk. Moisture from sweat or incontinence, poor nutrition, and friction from bed linens can all make things worse.
Pressure Ulcer Staging: What Each Stage Means
The National Pressure Injury Advisory Panel (NPIAP) uses a staging system to classify pressure ulcers by how deep the tissue damage goes. As an LPN, you need to know these stages well.
Stage 1: Non-Blanchable Redness
The skin is intact but there is redness that does not go away when you press on it. In patients with darker skin tones, the area may appear discolored, warm, or firm rather than red. No open wound yet, but this is your warning sign.
Stage 2: Partial Thickness Skin Loss
The top layers of skin — the epidermis and part of the dermis — are broken. It may look like a shallow open sore, a blister, or a shiny wet area. There is no visible fat or deeper tissue at this stage.
Stage 3: Full Thickness Skin Loss
Now the wound goes deeper, through all layers of skin and into the fat tissue underneath. You may see a crater-like wound. Slough (dead yellowish tissue) may be present. Bone, tendon, and muscle are not yet visible.
Stage 4: Full Thickness Tissue Loss
This is the most severe stage. The wound extends to muscle, bone, or supporting structures. There is significant risk of infection, including bone infection (osteomyelitis). These wounds require intensive, often specialized care.
Unstageable Wounds
When the wound bed is covered with enough slough or eschar (hardened dead tissue) that you cannot see how deep it goes, the ulcer is classified as unstageable. The stage cannot be confirmed until the dead tissue is removed.
Deep Tissue Pressure Injury
This one looks deceptively mild from the outside. The skin may be intact or only slightly broken, but there is deep bruising or a dark maroon or purple discoloration. Inside, the tissue is already significantly damaged. These can deteriorate rapidly.
How to Assess Skin Integrity on Your Rounds
Skin assessment should happen on every shift, especially for at-risk patients. Look at the whole body, not just the obvious areas.
Use a validated tool like the Braden Scale to score each patient’s risk level. It measures sensory perception, moisture, activity, mobility, nutrition, and friction. The lower the score, the higher the risk.
Document what you find accurately and report changes to the supervising nurse or provider immediately. A Stage 1 that gets missed becomes a Stage 2 by next shift.
Prevention: The Most Important Part of Your Job
Most pressure ulcers are preventable. Here is what evidence-based prevention looks like in practice.
Repositioning: Turn and reposition bedbound patients at least every two hours. For wheelchair users, offload pressure every 15 to 30 minutes. Use a turning schedule and document it.
Support Surfaces: Pressure-redistributing mattresses and cushions reduce the load on bony areas. Know what equipment your facility uses and when to request upgrades for high-risk patients.
Skin Care and Moisture Management: Keep skin clean and dry. Use barrier creams for patients with incontinence. Moisture softens the skin and increases breakdown risk significantly.
Nutrition: Adequate protein, calories, and hydration all support skin integrity. Flag patients who are not eating well for a dietitian referral.
Friction and Shear Reduction: Use draw sheets or slide boards when repositioning. Avoid dragging patients up in bed — this creates friction that damages the outer skin layers.
Understanding the Body Behind the Wound
To truly understand why pressure ulcers develop and progress, it helps to understand the structure of the skin and how tissue responds to reduced blood flow. Students who have completed anatomy and physiology classes before their nursing training often find wound care concepts easier to grasp in clinical rotations. Knowing the layers of the skin — epidermis, dermis, subcutaneous tissue — gives you a mental map when you are staging a wound.
The LPN’s Role in Wound Care
LPNs are on the front lines of pressure ulcer prevention and monitoring. Your role typically includes performing skin assessments, implementing and documenting prevention measures, applying wound dressings under the care plan, and reporting changes to the RN or provider.
You are not typically the one making the initial treatment plan, but you are the one who catches problems early. That makes your attention to detail one of the most important factors in patient outcomes.
Conclusion
Pressure ulcer staging and prevention is one of those skills that separates a careful nurse from a great one. The stages give you a clinical language to describe what you are seeing. The prevention strategies give you the tools to stop damage before it starts. And your consistent, attentive assessment is what connects both.
If you are working toward a nursing career and want to build these skills in a hands-on, structured environment, Verve College’s accredited lpn programs train students in exactly these kinds of real-world clinical competencies. This is the work that matters — and it starts with learning it right.
Get Your Nursing Career Training Readiness Score Now!
FAQs
- What is the difference between a Stage 3 and Stage 4 pressure ulcer?
A Stage 3 ulcer involves full thickness skin loss that reaches into the fat layer, but bone, muscle, and tendon are not visible. A Stage 4 goes all the way to those deeper structures. Stage 4 wounds carry a higher risk of serious complications like bone infection and require a more intensive level of care.
- Can a pressure ulcer heal and move back through the stages?
No. Staging only moves in one direction to describe the depth of tissue damage. As a wound heals, you do not re-stage it downward. Instead, you document it as a healing Stage 3 or Stage 4, for example. The stage reflects the original depth of damage, not the current state of healing.
- How do I know if I am learning wound care the right way in my nursing program?
Look for programs that include clinical rotations and hands-on skills training, not just classroom instruction. Wound care, skin assessment, and patient safety should be part of the curriculum. Ask about how clinical hours are structured and what skills you will practice before graduation.
 Sign up
Sign up Login
Login