- Oak Brook:(630) 705-9999
- Chicago:(312) 920-8822
- Email:inquiry@vervecollege.edu
- Make a Payment
- Home
- Programs
- Admission
- Resources
- ATI Entrance Exam Resources
- New E-Digital Library
- Refer a Friend
- School Newsletter
- Events
- Employers
- Job-Network
- Alpha Beta Kappa Candidates
- Verve College Library
- Graduation and Pinning Ceremony Photo Galleries
- Textbook Information
- Career Services
- Tutoring
- School Catalog
- FAQ
- Constitution Day Program
- Alumni
- Verve College Plans
- Financial Aid
- HEERF Reporting
- Satisfactory Academic Progress
- Apply For Financial Aid
- Net Price Calculator
- Return of Title IV Funds (R2T4)
- Financial Aid Office Code of Conduct
- Contact
- FAQs
- Verification Policy
- Vaccination Policy
- Student Right-to-Know Act
- Misrepresentation
- Information Security Program
- Academic Award Year
- Availability of Employee
- Cost of Attendance
- Health & Safety Exemption Requirement
- Students Rights and Responsibilities
- Leave of Absence
- Pell Formula
- Military Students
- Grants/ Scholarship Policy
- Contact Us
- Testimonials
- Blog
Is a Nursing Career Right For You?
Take The Free Quiz
What Is Cultural Competency in Healthcare?
What Is Cultural Competency in Healthcare?
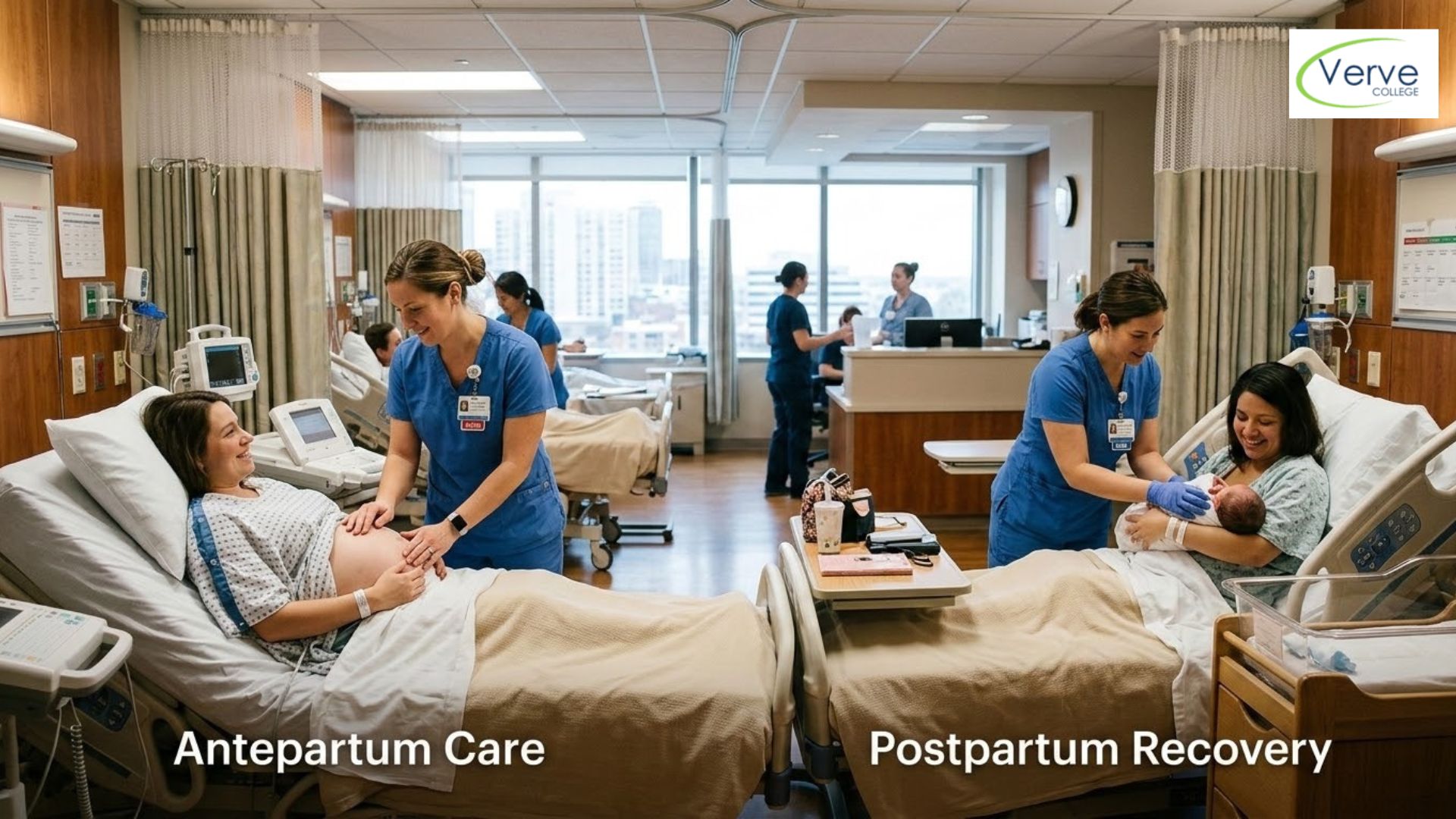
Walk into any hospital, clinic, or nursing home in Illinois, and you will immediately notice one thing: patients come from everywhere. Different countries, different languages, different beliefs about the body, illness, and healing.
Cultural competency in healthcare is the ability of a nurse or healthcare provider to understand, respect, and respond to those differences in a way that improves patient care. It is not a soft skill you pick up after graduation. It is something every nursing student needs to start building from day one.
This blog explains what cultural competency actually means in practice, why it matters more than most people realize, and how it shapes the kind of nurse you become.
Key Takeaways
- Cultural competency means understanding how a patient’s background affects how they experience illness and interact with healthcare providers
- It is a required part of quality, patient-centered care and not an optional add-on to clinical skills
- Nurses who practice cultural competency build more trust with patients, which directly improves health outcomes
- Verve College’s practical nursing program prepares students to care for diverse patient populations across real Illinois healthcare settings
- If you need a flexible path into nursing, the online hybrid practical nursing program offers the same quality preparation with more scheduling freedom
- Understanding the science of the human body through anatomy and physiology prep classes is foundational, but understanding the person inside that body is equally important
What Does Cultural Competency Actually Mean?
The term sounds formal, but the concept is straightforward.
Cultural competency is the ability to recognize that your patient’s cultural background shapes how they think about sickness, pain, treatment, and trust. It means adjusting how you communicate, how you explain a diagnosis, and how you approach care based on who the person in front of you actually is.
It is not about memorizing facts about every culture. No one expects that. It is about developing the awareness to ask the right questions, listen without assumptions, and adapt without judgment.
A culturally competent nurse notices when a patient seems reluctant to share information and considers whether a cultural or language barrier might be the reason. They do not assume the patient is simply uncooperative.
Why It Matters More Than You Might Think
Cultural differences directly affect patient outcomes. This is not a theory. It is backed by decades of healthcare research.
Patients who feel misunderstood or disrespected by their healthcare providers are less likely to follow treatment plans, less likely to return for follow-up care, and less likely to be honest about their symptoms. That breakdown in trust has real consequences for their health.
Language barriers are one piece of this. But cultural competency goes further. It includes understanding how a patient’s religion might affect their willingness to accept certain treatments. It means knowing that some patients come from communities where discussing illness openly is considered taboo. It means recognizing that pain is expressed differently across cultures, and that a quiet patient is not necessarily a comfortable one.
In Illinois, where Chicago alone is home to residents from over 130 countries, these situations are not rare exceptions. They are everyday realities for working nurses.
The Four Core Areas of Cultural Competency in Nursing
Cultural competency is not one single skill. It builds across several areas over time.
Cultural Awareness
This is where it starts. Cultural awareness means acknowledging that your own background shapes your assumptions and that other people’s experiences are just as valid, even when they are different from yours.
For a nursing student, this means examining your own biases before you walk into a patient’s room. Everyone carries assumptions. The difference is whether you examine them or act on them without thinking.
Cultural Knowledge
Cultural knowledge means learning about the health beliefs, practices, and values of different communities. Not to stereotype, but to understand context.
For example, some patients from certain cultural backgrounds prefer family members to be involved in medical decisions rather than speaking directly to the provider. Knowing this helps a nurse navigate those conversations with respect rather than confusion.
Cultural Skills
This is the practical side. Cultural skills involve conducting a patient assessment in a way that is sensitive to the patient’s background. It includes asking open-ended questions, using professional interpreters when needed, and adjusting your communication style without compromising clinical accuracy.
Cultural Encounters
You build real cultural competency through experience, not just study. Every patient interaction is a cultural encounter, and each one teaches you something a textbook cannot. This is why clinical training is so important in nursing education.
How Cultural Competency Shows Up in Daily Nursing Tasks
It is easy to think of cultural competency as something that only comes up in dramatic situations. In reality, it shows up in small moments throughout every shift.
It appears when a patient declines a medication and you take the time to understand why rather than simply documenting refusal. It shows up when a family member asks to be present during a procedure and you find a way to accommodate that request within the facility’s guidelines.
It is present when you ask a patient how they prefer to be addressed instead of assuming. It is there when you use plain language with a patient who seems overwhelmed by medical terminology, regardless of where they are from.
These are not extraordinary acts. They are the baseline of good nursing care. Cultural competency is what makes them consistent rather than occasional.
What Gets in the Way of Culturally Competent Care
Even well-intentioned nurses can fall into patterns that undermine cultural competency without realizing it.
One of the most common barriers is making assumptions based on appearance. A patient who speaks English fluently may still hold deeply rooted cultural beliefs about illness that differ from standard Western medical approaches. Fluency in language does not mean alignment in worldview.
Another barrier is time pressure. Nursing shifts are busy, and it can feel easier to follow a standard script than to slow down and individualize care. Culturally competent nursing requires a deliberate habit of pausing and checking in, even when the shift is moving fast.
Implicit bias is also a real factor. Research consistently shows that implicit bias affects clinical decision-making in ways providers are often unaware of. Recognizing this is not about guilt. It is about commitment to better care.
How Nursing Education Builds This Skill
Cultural competency is not something you either have or do not have. It is developed through education, reflection, and practice.
Good nursing programs weave cultural competency into the curriculum rather than treating it as a standalone topic. It comes up in pharmacology when discussing how different populations metabolize medications differently. It comes up in patient communication training. It comes up in mental health nursing when exploring how different cultures conceptualize psychological distress.
The real test of cultural competency comes during hands-on patient care. Learning what to expect from clinical externships for nursing students can help you understand how these skills are applied in real healthcare settings, where every patient brings a different background and a different set of needs.
Conclusion
Cultural competency is not a box to check. It is a practice that grows throughout your entire nursing career. The nurses who do it well are the ones patients remember, trust, and return to. They are also the ones who produce better health outcomes, not because they are more technically skilled, but because they treat the whole person and not just the condition. If you are preparing for a nursing career in Illinois and want a program that takes this seriously, Verve College’s practical nursing program is built around preparing you for the real, diverse, and deeply human work of patient care.
Get Your Nursing Career Training Readiness Score Now!
FAQs
Is cultural competency the same as cultural sensitivity?
They are related but not identical. Cultural sensitivity is the awareness that cultural differences exist and that they matter. Cultural competency goes a step further. It is the ability to act on that awareness in a clinical setting, adjusting how you communicate and deliver care based on a patient’s background. Sensitivity is the mindset. Competency is the skill.
What if I do not speak a patient’s language during a clinical placement?
You are not expected to speak every language. Healthcare facilities are required to provide professional interpreter services for patients with limited English proficiency. Your role as a nursing student is to recognize when a language barrier exists, advocate for the use of an interpreter, and avoid relying on family members to translate medical information, as this raises accuracy and privacy concerns.
How do I start building cultural competency before I graduate?
Start by reflecting honestly on your own assumptions and what shaped them. Read about the communities you are likely to serve in your region. Practice asking open-ended questions. And choose a nursing program that places you in diverse clinical settings early. If you are still building your prerequisites, beginning with anatomy and physiology prep classes is a practical first step, and the preparation for understanding diverse patients starts well before your first clinical day.
 Sign up
Sign up Login
Login